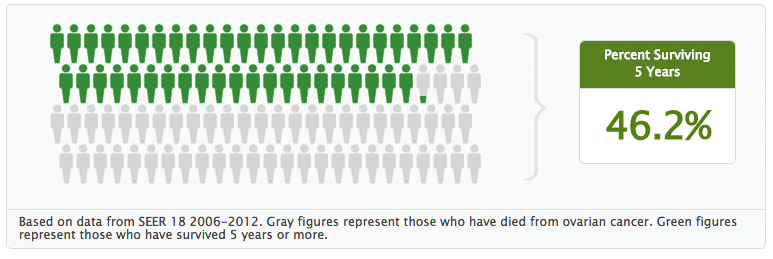
Ovarian cancer is ranked as the fifth highest mortality rate among women in the United States, with an estimated 22,440 new cases expected to be diagnosed in 2017. Often found at advanced stages, the SEER Program of the National Cancer Institute reports that the 5-year survival rate stands at only 46.2%
The question then becomes, what can we do to protect ourselves and our loved ones? The biggest problem currently faced by women is the lack of information, and of the amount of incorrect information that has been accepted. For example, most women are confident in knowing that maintaining a regular PAP test will ensure they are being screened for gynecological cancers. The truth is that while the PAP can detect abnormal cervical cells, it does NOT screen for Ovarian Cancer!
In fact, there are no reliable screening tests currently in existence. While some companies will claim they have a reputable test available, the U.S. Federal Drug Agency (FDA) announced in September 2016 that women should not put their faith in any tests that are currently marketed as screening tests for Ovarian Cancer. The Agency states, “there are currently no screening tests for Ovarian Cancer that are sensitive enough to reliably screen for ovarian cancer without a high number of inaccurate results.”
The current diagnostic process begins with three separate tests; a complete pelvic exam, a transvaginal or pelvic ultrasound and a CA-125 blood test. Using these tests in combination has proven to be the most effective. In the event that the doctor still has questions, they may choose to also order a CT scan or PET scan. In the end, the only definitive way to diagnose ovarian cancer is through a biopsy.
What Factors Increase Your Risk of Ovarian Cancer?
- Age: the risk of ovarian cancer increases as you get old, with the highest risk age group being women aged 50-79
- Family History: if you have any close blood relatives who have either been diagnosed with ovarian cancer at any age, or breast cancer prior to the age of 50, your risk is higher
- Ethnicity: Jewish women of Eastern European descent have a higher risk. Certain groups of French Canadians may also carry a higher risk; the studies are still being conducted to confirm this finding
- Oral Contraceptives/Hormone Replacement: if you have used oral contraceptives you have a lower risk, however if you have taken hormone replacement, regardless of the reason for having done so, this increases your risk
- Reproductive History: your risk is increased if you have not delivered a child, or if you have a history of difficult getting pregnant
- Endometriosis: if you have previously been diagnosed with endometriosis, this also increases your risk of ovarian cancer
Women Should Watch for These 4 Early Warning Signs:
- Pain – Whether in the pelvic or abdominal areas, any pain that is different than your usual menstrual cramping, or that lasts longer than 3 weeks, should warrant a conversation with your doctor
- Urinary Symptoms – Changes in the urgency or frequency of urination are a sign that something is off in your body. If you notice either that you need to urinate more often, or that you are starting to regularly feel a sudden and immediate need to urinate, consider that a red flag.
- Bloating – Persistent bloating, regardless of what you are eating, that you cannot seem to shake. This also includes if you notice an increase in the size of your abdomen with no explanation, even if you are not feeling like you are bloating at the time.
- Changes in Eating Habits – While these signs could indicate several different conditions, a change in your eating habits, combined with any of the above symptoms, is a cause for concern. These changes may include difficulty eating, or finding that you feel full quickly.
As the disease progresses, you may see additional signs and symptoms, including:
- Fatigue
- Heartburn
- Indigestion
- Menstrual irregularities
- Painful intercourse
- Constipation
- Back pain
